When you start saying “Back when I was in training…”, you are officially old.
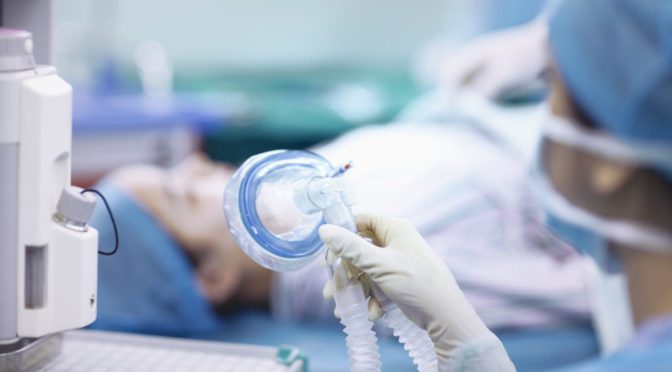
Well, back when I was in training, I didn’t think regional anesthesia was a career path. We weren’t using ultrasound yet, and catheters were still experimental. Regional anesthesia was just part of anesthesiology, and there was a fairly limited set of blocks to offer patients. Besides spinals and epidurals, I was fortunate to learn how to do more peripheral techniques than most residents in my cohort: the femoral nerve block; proximal and distal sciatic nerve block; brachial plexus blocks (interscalene, infraclavicular, and axillary); and paravertebral block. All of these blocks were performed using landmarks to guide needle placement, and we used indirect needle tip position endpoints for confirmation (e.g. nerve stimulation or paresthesia).
Fast forward to today, and the subspecialty field of regional anesthesia and acute pain medicine (RAAPM) has exploded! The demand for better perioperative pain control that doesn’t depend solely on opioids has driven the development of advanced clinical fellowships in RAAPM for anesthesiologists who want to become acute pain medicine experts. A consortium of 14 medical organizations representing anesthesiology, pain medicine, surgical specialties, and hospitals has unanimously agreed on a set of principles to guide acute perioperative pain management, and included in these principles is access to a pain medicine specialist and the employment of multimodal analgesia with regional anesthesia techniques when indicated.
What does this mean for medical students and anesthesiology residents who are thinking about their careers? The future of RAAPM is bright! Considering that physicians work for about 30 years or more after completion of training, it’s really important to find a specialty, and even a subspecialty, that: 1) allows you to take good care of patients and be the kind of doctor you’ve been called to be; and 2) continues to evolve in innovative ways so you can keep learning new and exciting things.
I’ve written before about how much I love being an anesthesiologist, but I really love being a RAAPM subspecialist! There is nothing more satisfying than preventing and treating pain for patients who are undergoing surgery or suffering from traumatic injury. Today’s RAAPM fellowship curriculum trains anesthesiology residency graduates over the course of one year to become leaders with the knowledge and skills to perform a wide range of advanced procedures and manage acute pain services in any practice setting. New procedures to extend the benefits of regional analgesia beyond the first few postoperative days are currently being studied, as are new models of care such as transitional pain services that can add significant value to healthcare systems.
After fellowship is over, you join an incredible worldwide community of RAAPM experts who will support and mentor you throughout your career. Conferences feel like family reunions, and the leaders in the field whom you’ve looked up to become your friends.
To learn more about our RAAPM fellowship at Stanford, please visit our website. Information on other programs is available through ASRA Pain Medicine.